Many people assume that when a toenail starts lifting away from the skin underneath, it must be a fungal infection. Surprisingly, this is often not the case.
A detached toenail, known medically as onycholysis, can occur for many different reasons. While fungal infections can sometimes cause nail separation, many patients have repeated fungal tests that come back completely clear. In these cases, the cause is often mechanical rather than infectious.
What Does Toenail Separation Look Like?
The nail may begin separating from:
- The inside (medial) border of the nail
- The outside (lateral) border of the nail
- The tip of the nail (distal edge)
- Multiple borders at the same time
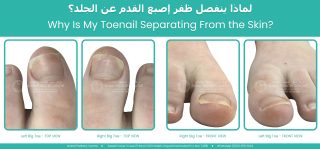
In severe cases, the entire nail plate may become detached from the nail bed, leaving the nail attached only at the nail root.
Cause #1 – Repetitive Pressure From Footwear
One of the most common causes of nail separation is repeated pressure from footwear.
This can occur when:
- Shoes are too short or too narrow
- The toe repeatedly hits the front of the shoe
- The toe hyperextends upward and strikes the roof of the shoe
When the toenail is repeatedly compressed, the tissues beneath the nail become irritated and swollen. As the swelling settles, the connection between the nail plate and the nail bed can weaken, causing the nail to lift away from the skin.
A useful clue is the appearance of horizontal ridges across the toenail. These ridges run from side to side and often indicate repetitive trauma from the toe repeatedly striking the shoe.
Cause #2 – Aggressive Cleaning Under The Nail
Many people regularly clean underneath their toenails using nail files, scissors, metal instruments, or other sharp tools.
Unfortunately, this can gradually separate the nail from the skin underneath.
In fact, when podiatrists remove a toenail surgically, one of the techniques involves releasing the nail from the nail bed using specialised instruments. Excessive cleaning under the nail can unintentionally create the same process over time.
The more the nail is lifted and cleaned underneath, the easier it becomes for the separation to progress.
Cause #3 – Abnormal Toe Position and Foot Mechanics
Perhaps the most surprising cause of toenail separation is abnormal toe movement during standing and walking.
This is often the most overlooked cause and, in many cases, the most common.
When the foot collapses inward, the arch flattens, or a bunion develops, the toe is no longer functioning in a neutral position.
The toe may:
- Rotate inward or outward
- Drift sideways
- Move excessively forward
- Twist during walking
When this happens, the soft tissue beneath the nail is repeatedly pulled and stretched.
Rather than the nail being pushed away by pressure from above, the skin underneath is gradually pulled away from the nail by repetitive micro-trauma.
Over thousands of steps each day, the tissues can slowly detach from the nail plate.
For example:
- If the ankles lean inward and the big toe rotates, separation commonly develops along the outer border of the big toenail
- If a bunion causes the toe to drift sideways, tension can develop on one side of the nail bed
- If the toes spread excessively due to arch collapse, the tissues beneath the nail can be repeatedly stretched and irritated
The result can look very similar to a fungal nail infection, even when no fungus is present.
Why Standing Examination Matters
Many nail problems are missed because the feet are examined only while the patient is sitting.
The position of the toes can change dramatically once a person stands and begins walking.
A proper assessment should include:
- Standing examination
- Walking analysis
- Heel raise testing
- Observation of toe-off during gait
- Assessment of foot posture and ankle alignment
Only then can the true cause of the nail separation be identified.
Examining The Shoes
The footwear often provides valuable clues.
We frequently examine:
- The original insoles
- Wear patterns inside the shoe
- Pressure marks from the toes
- Areas where the toes slide forward
Older shoes are often more useful because they clearly show where pressure has been occurring over time.
One particularly revealing finding is damage to the inner roof of the toe box. In some cases, the fabric lining has been worn away by the toenail repeatedly striking the ceiling of the shoe during walking.
This provides clear evidence that the nail is being traumatised from above.
The Importance Of Finding The Real Cause
Treating a detached toenail successfully requires identifying why the nail is separating in the first place.
If the cause is fungal, antifungal treatment may be required.
However, if the cause is mechanical, treatment should focus on correcting the underlying problem, such as:
- Footwear modification
- Orthotic therapy
- Correction of abnormal foot posture
- Management of bunions
- Reduction of excessive toe movement
- Protection of the nail from repetitive trauma
Without addressing the underlying cause, the nail may continue to separate regardless of how many creams, sprays, or antifungal treatments are used.
At Dubai Podiatry Centre, we assess not only the nail itself but also the biomechanics of the foot and the forces acting on the toe during standing and walking. Understanding these forces is often the key to solving long-standing nail problems that have been mistakenly attributed to fungal infection.
For more information or to book an appointment please call our clinic +971 4 3435390 or WhatsApp +971 50 3553024


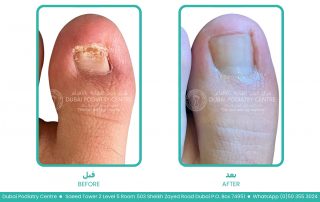
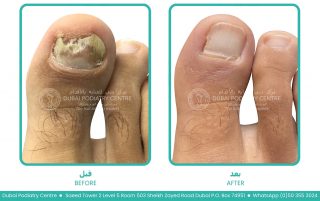
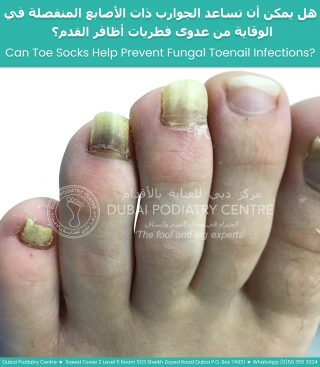 When the toes are squeezed together for long periods, moisture becomes trapped and air circulation is reduced. This creates the perfect environment for fungal spores to grow and spread. Over time, the infection may remain confined to the skin between the toes, or it may spread into the neighbouring toenails, particularly the fourth and fifth toenails, resulting in fungal nail infection (onychomycosis).
When the toes are squeezed together for long periods, moisture becomes trapped and air circulation is reduced. This creates the perfect environment for fungal spores to grow and spread. Over time, the infection may remain confined to the skin between the toes, or it may spread into the neighbouring toenails, particularly the fourth and fifth toenails, resulting in fungal nail infection (onychomycosis).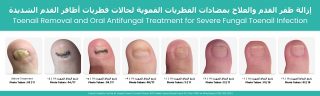
 At Dubai Podiatry Centre, our highest success rate for plantar warts comes from our Dermojet treatment.
At Dubai Podiatry Centre, our highest success rate for plantar warts comes from our Dermojet treatment.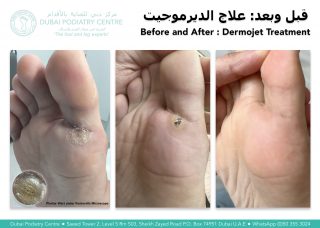

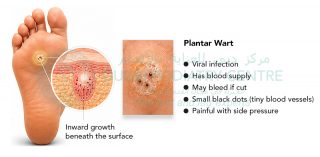
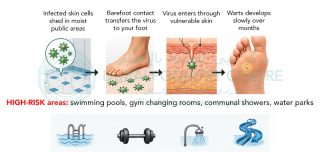 The condition is caused by a virus that is spread through contact with infected skin cells. This typically occurs in high-risk environments where people walk barefoot, such as swimming pools, gym changing rooms, and water parks. An infected skin cell from another person can be shed onto the floor, and if you walk over that area within a short time frame, the virus may transfer to your foot.
The condition is caused by a virus that is spread through contact with infected skin cells. This typically occurs in high-risk environments where people walk barefoot, such as swimming pools, gym changing rooms, and water parks. An infected skin cell from another person can be shed onto the floor, and if you walk over that area within a short time frame, the virus may transfer to your foot.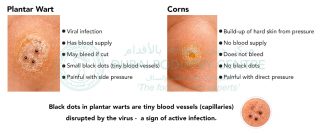 Plantar warts are sometimes confused with corns, but they are very different. A corn is a build-up of hard skin caused by pressure and friction. It can often be reduced without bleeding, although it may feel like walking on a sharp point. A plantar wart, however, is a living viral lesion. If disturbed or cut, it will bleed because it has developed its own blood supply within the skin.
Plantar warts are sometimes confused with corns, but they are very different. A corn is a build-up of hard skin caused by pressure and friction. It can often be reduced without bleeding, although it may feel like walking on a sharp point. A plantar wart, however, is a living viral lesion. If disturbed or cut, it will bleed because it has developed its own blood supply within the skin.